Pain in the shin is one of the most common overuse complaints in everyday sports orthopaedics. It particularly affects physically active people whose shin structures become overloaded due to intense or unfamiliar training demands. The symptoms can significantly limit performance and may require longer breaks from training. This makes an early orthopaedic assessment all the more important. With comprehensive diagnostics and individually tailored treatment approaches, so-called shin splints can be treated effectively in most cases. Below, you will learn how we can support you in reducing your symptoms and safely returning to your sporting activity.

What are shin splints?
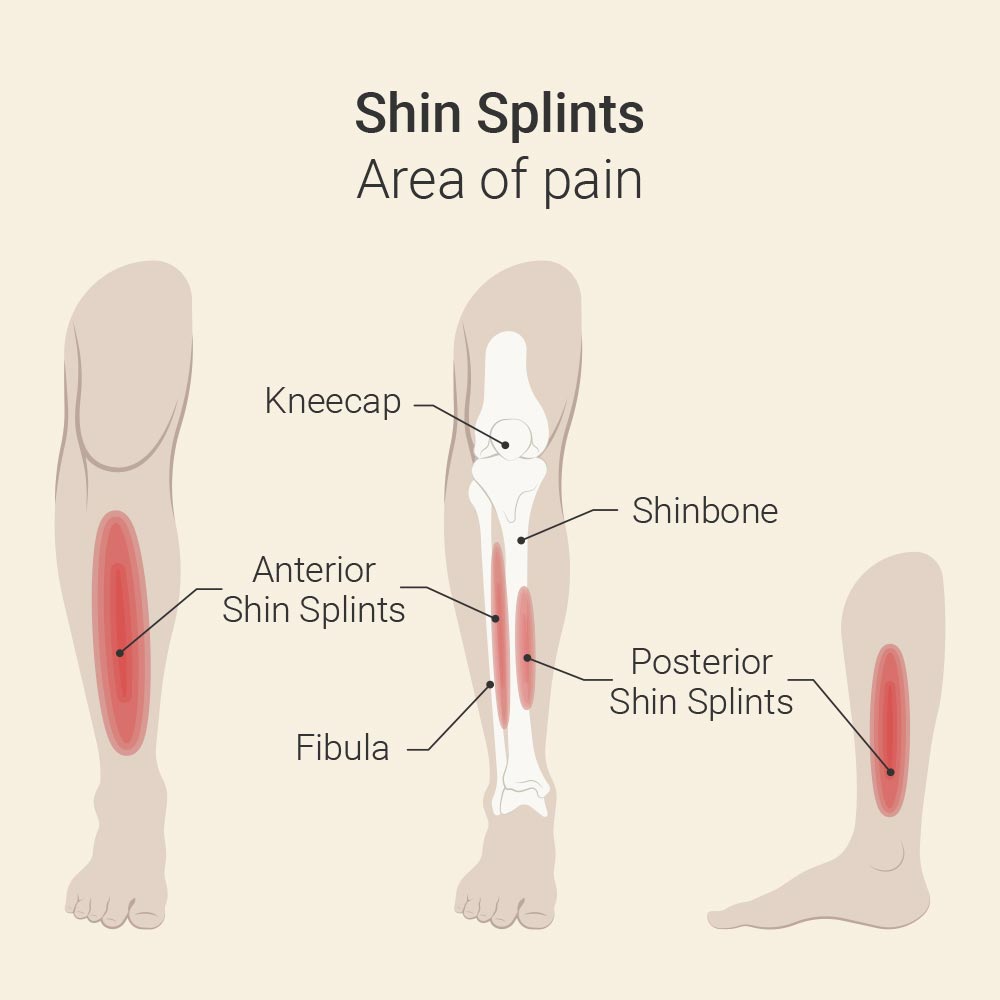
If you experience pain along the shin while running or jumping, the cause may be a condition known as medial tibial stress syndrome, also commonly referred to as shin splints. Typically, the symptoms occur along the inner edge of the shinbone and are especially common in physically active people. From an orthopaedic perspective, this is an overuse reaction of the structures around the shinbone, particularly the periosteum as well as the muscles and tendons that attach there.
The symptoms often develop gradually. At first, you may notice a slight pulling sensation during training, which becomes stronger over time or lasts longer. Common causes include excessive strain, a training load that increases too quickly, unsuitable footwear, hard surfaces or unfavourable individual movement patterns.
If the symptoms are ignored, the pain may no longer occur only during activity, but may also persist afterwards or at rest. As a result, shin splints can increasingly restrict your everyday life and your sporting activities.
How are shin splints diagnosed?
When you come to our private practice for orthopaedics and traumatology in Frankfurt with pain in the shin area, a precise assessment of your symptoms is our main focus. The aim is to accurately classify the cause of your complaints and rule out other possible conditions.
At the beginning, we talk with you in detail about your symptoms. Among other things, we discuss when the pain first occurred, what it feels like and in which situations it becomes more intense. Your training habits, possible increases in load, your footwear and the surface on which you train also play an important role.
This is followed by a physical examination. We palpate your shinbone to identify painful areas. In addition, we examine the surrounding muscles and tendon structures as well as your mobility and load capacity. A clearly localised pressure pain along the inner edge of the shinbone is typical of shin splints.
Further examinations are not necessary in every case. However, if bone involvement is suspected, such as a stress fracture, we use imaging procedures for further clarification.
Magnetic resonance imaging (MRI) provides a differentiated view of bones, muscles and tendons and can make overuse reactions visible at an early stage. In certain cases, a bone scintigraphy scan may also be useful to assess metabolic changes in the bone. An X-ray is mainly used to rule out structural changes or advanced findings.
This ensures that your symptoms are correctly classified and that you receive treatment tailored to your individual needs.
Differential diagnoses: Which conditions can cause symptoms similar to shin splints?
Even though the symptoms are often attributable to shin splints, various other orthopaedic causes may produce a similar pattern of complaints. Clear differentiation is essential because treatment can vary considerably depending on the diagnosis. In our practice in Frankfurt, we therefore make sure to identify possible differential diagnoses early and rule them out reliably.
The most important differential diagnoses include:
This is a fine bone injury, usually not completely continuous at first, that develops as a result of repeated overuse. The cause is generally excessive strain or a training load that increases too quickly, leaving the bone with insufficient time to regenerate.
In contrast to shin splints, the pain is usually very precisely localised to one point and can often be indicated exactly with a finger. It increases significantly under load and, as the condition progresses, may also occur at rest or at night. Load capacity is often considerably reduced, making sporting activities barely possible.
In chronic compartment syndrome, the pressure within the muscle compartments of the lower leg increases during exertion. This temporarily compresses muscles, nerves and blood vessels, which triggers the symptoms. The cause is often repeated overuse, in which the muscles expand during activity but the surrounding tissue compartment does not yield sufficiently.
Typical signs include load-dependent pain, a pronounced feeling of tightness and, occasionally, numbness or tingling sensations. The symptoms usually occur repeatedly during specific forms of exertion and subside again during rest phases.
Overuse of individual tendons in the lower leg can also cause symptoms similar to those of shin splints. Frequently affected, for example, are the tendons of the tibialis posterior or tibialis anterior muscles, which can become irritated through repeated strain.
Unlike shin splints, however, the pain can usually be clearly localised along the course of the respective tendon and typically occurs only during certain movements or forms of exertion.
Not every irritation of the periosteum at the shinbone is automatically caused by shin splints. Other forms of overloading or incorrect loading can also trigger such inflammation, for example unfamiliar movement patterns or one-sided loading patterns.
The symptoms often resemble those of shin splints, but they cannot always be clearly assigned to the typical edge of the shinbone and therefore require a differentiated orthopaedic assessment.
In rarer cases, circulatory disorders or nerve irritation in the lower leg can also cause similar symptoms. In these cases, the cause is not directly in the shinbone itself, but in the structures that supply the area.
Typical symptoms are more diffuse pain that cannot be clearly localised and is sometimes accompanied by tingling, numbness or a feeling of cold. A precise assessment is particularly important here in order to identify and treat the underlying cause.
Injuries to the lower-leg muscles can also cause symptoms that initially resemble shin splints. These mainly include muscle strains or minor muscle fibre tears, which usually occur in connection with acute overuse or sudden peaks in strain.
Unlike shin splints, the pain often begins more suddenly and can frequently be linked to a specific incident or moment during training. It is also usually limited to a specific muscle area and increases when the affected muscle is actively tensed.
Treating shin splints: What you can do yourself for shin pain
Once the diagnosis of shin splints has been confirmed, there is a lot you can do yourself to get the symptoms under control. With the right measures, you can relieve the affected structures and actively support healing. The key is to recognise overload factors early and reduce them consistently.
This creates the basis for lasting freedom from symptoms:
Give your shinbone enough time to regenerate. This does not necessarily mean complete inactivity, but it does require a clear adjustment of your training intensity. In particular, temporarily avoid running and jumping loads that may worsen the symptoms.
Cold applications can help reduce pain and calm inflammation. Cool the affected area several times a day for a few minutes, for example with a cold pack.
Specific stretching and strengthening exercises play a central role in relieving the shinbone. To ensure that you target the right muscle groups and avoid incorrect loading, individual guidance from physiotherapy professionals is recommended. They will show you exercises tailored to your symptoms and help you avoid incorrect strain. Training at the gym can also be a useful addition. However, this should only take place once you have mastered the exercises safely and train in a way that is adapted to your symptoms.
To maintain your fitness, it may make sense to temporarily switch to sports that are easier on the joints. Activities such as cycling or swimming allow you to stay active without further irritating the shinbone.
Make sure you wear well-cushioned, stable sports shoes that suit your foot type. If malpositions are present, orthopaedic insoles can help correct incorrect loading and distribute strain more evenly.
Light self-massage, for example with a fascia roller, can promote circulation and reduce muscular tension in the lower leg. It is important to use it in a controlled way that does not cause pain.
As soon as the symptoms begin to subside, you can gradually and carefully resume your usual training. However, be cautious: returning too quickly to your original training level significantly increases the risk of the symptoms recurring.
The importance of physiotherapy for shin splints
Physiotherapy is a central component of treatment and crucial for lasting freedom from symptoms. It addresses the causes of overuse and helps identify and correct incorrect loading.
Through individually tailored exercises, the muscles, mobility and load capacity of the lower leg are gradually improved. Manual techniques may also be used to release tension and relieve the affected structures.
Treating shin splints: Additional options with Dr. Tabrizi in Frankfurt
With Kinesio taping, we apply elastic, skin-friendly tapes along the affected muscle and tendon pathways. The aim is to influence the mechanical load in the shin area and reduce tensile forces on the periosteum. At the same time, the tape can regulate muscle tension through sensory stimuli and improve body awareness, which may have a positive effect on movement patterns.
Kinesio tapes are mainly used as a supportive measure. Many patients experience noticeable relief, particularly in the acute phase, and benefit from increased stability in the affected area.
Correct application technique is important, however, as the effect depends strongly on the individual situation and exact placement. In addition, taping should always be embedded in a holistic treatment concept.
More about this: Kinesio taping in Frankfurt
Acupuncture is a procedure from traditional Chinese medicine in which fine needles are placed at specific points on the body. The treatment can relieve pain, regulate muscular tension and activate the body’s own healing processes.
In an orthopaedic context, acupuncture can be used especially for shin splints to reduce load-related pain and relax the muscles in the lower leg. Many patients report relief from symptoms, particularly in cases of long-standing or recurring complaints.
Its effect is attributed, among other things, to improved circulation, the release of the body’s own pain-inhibiting substances and regulation of muscle tone.
It is important, however, that this method also does not directly eliminate the actual cause, namely the overuse of the structures around the shinbone. It is therefore used as a complementary measure within a holistic treatment concept, for example together with physiotherapy.
Extracorporeal shock wave therapy (ESWT) uses high-energy sound waves directed at the painful areas of the shinbone. They can stimulate tissue metabolism, improve circulation and activate healing processes.
Especially in cases of long-standing symptoms, shock wave therapy can help reduce pain and promote regeneration of the affected structures.
Here, too, it is important to note that shock wave therapy does not replace treatment of the underlying overuse, but complements it.
Treating shin splints in Frankfurt: Individual therapy for lasting freedom from symptoms
As you can see, shin pain is a common but very treatable condition, provided the cause is recognised early and treated accordingly. A holistic approach is essential, one that both relieves the acute symptoms and addresses the underlying overuse factors.
In our private practice for orthopaedics and traumatology in Frankfurt, this is exactly the approach we take. Based on careful diagnostics, we develop an individually tailored treatment concept for you that sensibly combines various therapeutic measures depending on the findings. Our experience shows that this can achieve significant symptom relief in most cases and enable a safe return to sporting activity.
Would you like to have your symptoms assessed or are you looking for suitable treatment? Then please feel free to book an appointment. As experts in the treatment of shin pain, among other conditions, we support you on your way back to greater resilience and enjoyment of movement.
1864549447 © Ratirat | 437441696 © Pepermpron| stock.adobe.com